Client profile
The organization operates in the health insurance sector, offering coverage plans and healthcare benefits to individuals and businesses. Their services focus on improving access to care while managing cost, compliance, and operational efficiency across insurance workflows.
With a global footprint and a large provider network, the company handles high volumes of claims, customer interactions, and partner coordination. Their operations depend on accuracy, timely claim processing, and coordinated communication across systems and teams.
Technical challenges
The client relied on multiple systems to manage claims, provider networks, fraud detection, and customer engagement. These systems operated in silos and lacked coordination, scalability, and automation. As demand increased, operational delays, inefficiencies, and limited visibility began to affect service quality and cost control.
Complex claims processing
High claim volumes required multiple manual review steps, which extended processing timelines and delayed approvals and payments across workflows.
Provider network visibility
A large network of hospitals and doctors made it difficult to maintain accurate records while keeping service availability current across locations.
Limited fraud detection accuracy
Existing systems could not consistently identify suspicious patterns, which meant fraudulent claims often went undetected and resulted in avoidable financial losses.
Personalization in engagement
Customer interactions lacked contextual insight, making it difficult to deliver relevant, personalized recommendations at scale.
Our solution
We designed and implemented a generative AI-led solution across claims processing, fraud detection, provider management, and customer engagement workflows. AI models were embedded into existing systems in stages, with each functional area built and validated before connecting into a unified system.
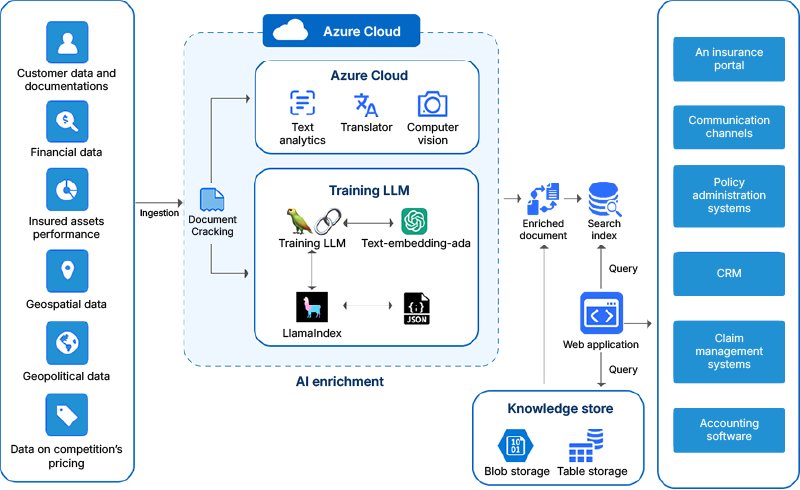
Data pipelines handled document processing, pattern analysis, and contextual data retrieval across the solution. Connection points across claims systems, CRM platforms, and provider data sources kept data flow and processing consistent throughout.
Intelligent claims processing with NLP and policy validation
We implemented an AI-driven claims processing system using natural language processing to extract structured data from claim documents. Extracted data ran against policy rules and validation logic, supporting automated claim assessment and clear exception identification.
Connection to existing claims systems kept processed data consistent with policy records and historical inputs. Flagged cases routed automatically to manual review queues, keeping exceptions within established operational processes.
AI-supported provider network visibility and coordination
We structured provider data into a centralized system to improve visibility across hospitals, doctors, and service records. AI-based classification and tagging helped organize provider information into consistent, structured datasets.
Provider data connected to internal systems so every update stayed consistent, regardless of where it originated. Access controls and data validation layers maintained accuracy and kept updates controlled at every entry point.
AI-driven fraud detection and anomaly identification
We deployed machine learning models to analyze historical claims data and identify patterns linked to fraudulent activity. Incoming claims are checked against these patterns, with anomalies and risk indicators flagged for the review team.
Model outputs fed directly into the claims workflow, giving reviewers structured signals on each flagged case. Data pipelines continue to feed new claim data into the models, keeping detection current as claim patterns shift.
Generative AI-powered customer recommendations and interactions
We integrated generative AI models with the client’s CRM platform to process customer data and generate contextual recommendations. Inputs such as demographic details, policy history, and risk profiles were used to define the recommendation logic.
The implementation aligned generated outputs with CRM workflows, ensuring that recommendations could be accessed within existing engagement processes. Data handling controls were applied to maintain consistency and security across customer interactions.
Data-driven asset management and investment insights
We extended generative AI capabilities into asset management workflows by integrating market data sources and historical datasets. The system processes these inputs to generate structured insights based on defined evaluation parameters.
Integration with internal financial systems ensured that generated insights remained aligned with existing data models. Data pipelines and validation steps were introduced to maintain consistency and support ongoing analysis.
We created a structured flow of data from Oracle and external sources into Snowflake. Along with this, we developed a detailed Standard Operating Procedure (SOP) for processing and transforming the data.
Our data team illustrated how and when data moved through staging servers and was handled by a Windows Scheduled Task and Console App. The SOP outlined each step—from data validation and transformation logic to error checks and load sequencing. Once processed, the data was stored in Snowflake and made available for reporting in Power BI.
Business goals & measurable outcomes
| Business objective | Business benefit delivered |
|---|---|
| Speed up claim approvals | Automated validation cut manual review steps, shortening approval timelines and making turnaround more consistent |
| Detect fraud before payout | AI models caught patterns that rule-based systems missed, reducing financial losses and sharpening investigator focus |
| Maintain provider accuracy | A centralized provider database reduced inconsistencies and gave teams a reliable, current view of network availability |
| Personalize at scale | Policy history and risk data shaped recommendations that improved interaction relevance and policy adoption |
| Cut manual processing effort | Automated workflows cut repetitive tasks across claims and engagement, freeing teams for exceptions and complex decisions |
| Support investment decisions | Market and historical data fed into a structured system, giving the asset team a reliable base for evaluating positions |
Tech Stack
- AI & Intelligence Layer:
- Generative AI, Large Language Models (LLMs), Natural Language Processing (NLP)
- Frameworks & Orchestration:
- LangChain
- AI Platform:
- Azure OpenAI Service
- Data Processing & Pipelines:
- Document Processing Pipelines, Data Extraction & Transformation
- Machine Learning:
- Predictive Modeling, Anomaly Detection (Fraud Detection Models)
- Integrations:
- Claims Management Systems, CRM Platforms, Provider Data Systems
- Automation & Workflow:
- AI-Driven Claims Processing, Rule-Based Validation, Automated Decision Workflows
- Architecture:
- AI-Powered Intelligent Automation Platform for Insurance Workflows
- Security & Governance:
- Secure Data Handling, Access Control, Compliance-Ready Data Processing
Similar case studies

Empowering wealth management operations with GenAI solutions

How our generative AI solution personalized the banking experience

Softweb redefined the traditional policy management for a leading insurance firm
Connect Now
Our experts would be eager to hear you.
